Andrew Siegel, MD 1/23/16
The word “robot” was coined by a Czech playwright almost a century ago, derived from “robota,” meaning “forced labor.” Now used routinely, robotics represents a significant engineering advance that has been rapidly adopted by urologists since its inception 15 years ago. Before the availability of this technological breakthrough, major urological surgical procedures were performed through large incisions with poorer visualization, more blood loss, less precision, more pain and longer hospital stays and recovery.
With the advent of laparoscopy (“keyhole”) surgery done via small portals and thereafter the development and refinement of surgical robotics, many advantages have accrued. Major surgical procedures can be performed less invasively, with a reduction in blood loss, a brighter, sharper and magnified visual field for the surgeon, less pain and faster recovery. The robot has been put to use for prostate, bladder, kidney and adrenal surgery as well as for severe cases of female pelvic organ prolapse. Robotic technology has been beneficial in helping urologists remove diseased organs as well as in facilitating reconstructive urological procedures. Robots do not perform the surgery independent of the surgeon! The urologist with a dedicated team of assistants harnesses the powers of the robot for the benefit of the patient, the robotic technology an extraordinary example of human-machine symbiosis.
Initially, portals are placed by small incisions that leave only small scars and cause limited pain. Through one of these portals, a camera is inserted to obtain an optically magnified, three dimensional, high definition view of the surgical field. The camera can be manipulated, zoomed, rotated, etc. Robotic instruments that are mounted on the robot’s arms are inserted through the portals. These include electric cautery used to cut and coagulate tissue, scissors, forceps, scalpels, needle holders and other surgical tools.

(The operative field with robotic instruments mounted on robotic arms)
The surgeon sits at a console remote from the patient and controls and maneuvers the miniaturized robotic instruments while viewing the operation in real time. An advantage of sitting at the console is that it is a very comfortable, ergonomically favorable position that minimizes the postural fatigue that often accompanies standing up for traditional open surgery. The surgeon’s fingers are inserted into surgical joysticks that provide control of the instruments by using natural hand and wrist movements, with the system capable of “motion scaling,” converting the surgeon’s movements to precise, tremor-free robotic micro-movements. In addition to hand controls the surgeon uses foot pedals to control the camera, focus, electro-cautery and coagulation. Seven degrees of freedom (each direction a joint can move is a degree of freedom) are provided at the instrument tips. 540 degrees of pivoting provide greater maneuverability than is possible with the human hands or laparoscopic instruments.
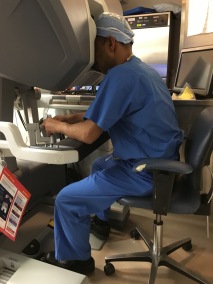
(Dr. Mutahar Ahmed seated at the console performing a robotic prostatectomy)
Robot-assisted laparoscopic prostatectomy is the surgical approach of choice for removing a cancerous prostate gland, allowing the surgeon the benefits of markedly better vision and maneuverability, very refined precision in the dissection of delicate tissue and facilitation of suturing. Because of these advantages, in addition to less bleeding, less post-operative pain and shorter hospital stays, there are improved outcomes in terms of urinary incontinence and erectile dysfunction as compared with the open approach.
Bottom Line: Surgical robotics is a revolutionary technological advance that has been rapidly adopted by urology, general surgery, gynecology, cardio-thoracic, pediatric and ear-nose-throat surgeons. It affords numerous advantages including surgeon comfort and ergonomics, high quality 3D vision, motion scaling, enhancement of surgeon dexterity and elimination of tremors, which translates to numerous benefits and advantages to the patient.
Exactly one year ago, New Jersey Center for Prostate Cancer & Urology (NJCPCU) and Bergen Urological Associates (BUA) merged practices. The main office is located at 255 W. Spring Valley Avenue in Maywood, New Jersey. The combined group consists of 8 urologists, a physician’s assistant and nurse practitioner. The merger brings together the exceptional robotic skills of the NJCPCU urologists (having pioneered robotic prostatectomy in New Jersey and having performed more than 7000 such procedures) with the urological expertise and experience of the BUA urologists.
RoboticUrology.com BergenUrological.com
Wishing you the best of health,
![]()
A new blog is posted every week. To receive the blogs in the in box of your email go to the following link and click on “email subscription”: www.HealthDoc13.WordPress.com
Author of Male Pelvic Fitness: Optimizing Sexual and Urinary Health: available in e-book (Amazon Kindle, Apple iBooks, Barnes & Noble Nook, Kobo) and paperback: www.MalePelvicFitness.com. In the works is The Kegel Fix: Recharging Female Pelvic, Sexual and Urinary Health.
Co-creator of Private Gym, a comprehensive, interactive, FDA-registered follow-along male pelvic floor muscle training program. Built upon the foundational work of Dr. Arnold Kegel, Private Gym empowers men to increase pelvic floor muscle strength, tone, power, and endurance: www.PrivateGym.com or Amazon.
Tags: Andrew Siegel MD, Bergen Urological, Christopher Wright MD, Greg Lovallo MD, laparoscopy, Martin Goldstein MD, Michael Esposito MD, Mutahar Ahmed MD, New Jersey Center for Prostate Cancer & Urology, radical prostatectomy, reconstructive urology, robotics, robotics in urology, surgical robotics, Thomas Christiano MD, urology, Vincent Lanteri MD
August 5, 2017 at 9:30 AM |
[…] to view the entire inside of the urinary tract, as well as ultrasound, lasers, laparoscopy and robotics. There is overlap in what urologists do with other medical and surgical disciplines, including […]